Prevention
Modern medicine is increasingly transitioning towards preventive care. This shift towards prevention has also been observed in breast cancer care in recent years, particularly with the discovery of the BRCA gene. Subsequently, multiple genes and risk factors have been identified. Depending on these factors, a personalized screening strategy can be chosen. Therefore, it is crucial to understand these genetic and risk factors.
Diagnosis
I was diagnosed with cancer ... This website serves as a portal designed to assist you and your loved ones in accessing personal information and finding solutions to your concerns.
The primary goal of this website is to offer guidance and support to patients as they navigate their journey toward recovery and improved quality of life. The "Diagnosis" section of our website is divided into two main categories. Firstly, under "Anatomy and Physiology," we provide fundamental knowledge about the breast. Secondly, in the "Tumors and Disorders" section, we delve deeper into various breast-related conditions.
Moreover, we aim to provide information to women who may be concerned about potential breast issues but are hesitant to seek immediate medical advice. Knowledge and information can often offer immediate reassurance if a woman is able to identify the issue herself and determine that no specific treatment is necessary. Conversely, we also strive to educate women who have received a diagnosis of a serious breast condition, such as breast cancer, and wish to approach their doctor well-informed and prepared.
Treatment
The treatment for breast cancer should immediately include a discussion about reconstruction. Our foundation has no greater goal than to raise awareness of this among patients and oncological surgeons. By making an informed decision beforehand, we avoid closing off options for later reconstruction while still considering the oncological aspect. Of course, survival is paramount, and the decision of the oncologic surgeon will always take precedence.
The "Reconstruction or not?" page contains all the information you can expect during an initial consultation before undergoing tumor removal. This page is comprehensive, and your plastic surgeon will only provide information relevant to your situation.
"Removing the tumor" details the surgical procedure itself. This is the most crucial operation because effective tumor removal remains paramount. We guide you through the various methods of removal, a decision often made by a multidisciplinary team comprising oncologists, radiologists, pathologists, radiotherapists, breast nurses, gynecologists, oncological surgeons, and plastic surgeons.
The "Breast Reconstruction" section includes information and illustrations of the different reconstruction options along with corresponding steps.
Revalidation
Those treated for cancer often need a long period to recover.
Cancer is a radical illness with a heavy treatment. Often, people have to deal with psychosocial and/or physical problems afterwards, such as stress, anxiety, extreme fatigue, painful joints, reduced fitness, lymphedema... This can have a major impact on general well-being.
There are rehabilitation programmes offered by most hospitals. We cover some of the major topics here.
Quality of life
Quality of life is a key factor in coping with breast cancer. Therefore, it is important to find coping mechanisms that work, which will be different from patient to patient. For some, it may be finding enjoyment in activities they engaged in prior to diagnosis, taking time for appreciating life and expressing gratitude, volunteering, physical exercise... Of prime importance, studies have shown that accepting the disease as a part of one’s life is a key to effective coping, as well as focusing on mental strength to allow the patient to move on with life. In this section we are addressing some topics that patients experience during and after treatment and we are providing information to address them.
Reconstruction or not?
Is breast reconstruction always necessary?
Breast reconstruction is not always necessary since considerable improvements have been made in the ablative procedures. In contrast to the highly aggressive methods at the beginning and middle of the last century, when large portions of the breast and chest wall were removed (fig. 1, Halsted procedure), in recent years, there has been a trend towards less aggressive mastectomies (fig. 2, modified radical mastectomy) and more limited resections.
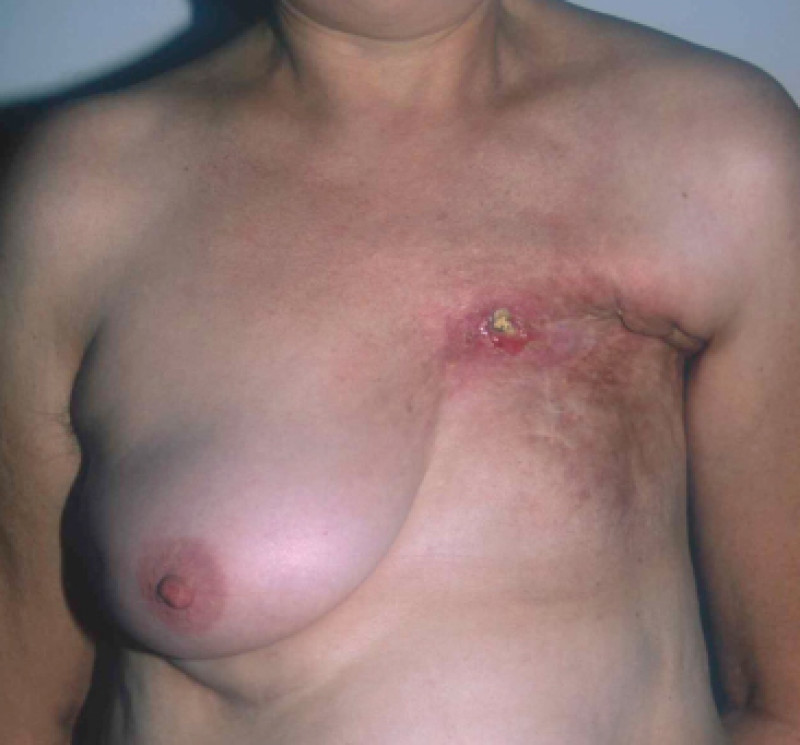
Fig. 1 Halsted procedure
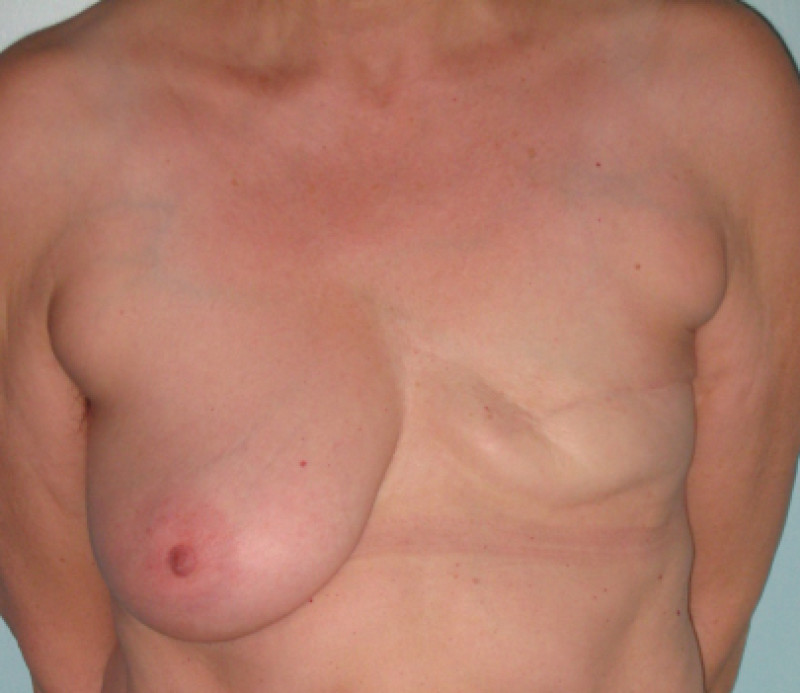
Fig. 2 Modified radical mastectomy
These more limited resections are referred to as “breast-conserving surgery” or “breast conservative therapy”: only a small segment of the breast is removed and the remaining breast is irradiated (tumorectomy or segmentectomy). In some cases an acceptable aesthetic result can be achieved (fig. 3), but if patients are very sensitive to irradiation, the scarring and fibrosis of the remaining gland and overlying skin can cause a significant breast deformity (fig. 4). In addition, breast conserving surgery cannot be performed in all patients. In individuals with a small breast, or those who have a large tumor, a mastectomy remains the gold standard and frequently better results can be achieved when a mastectomy is combined with an immediate breast reconstruction.
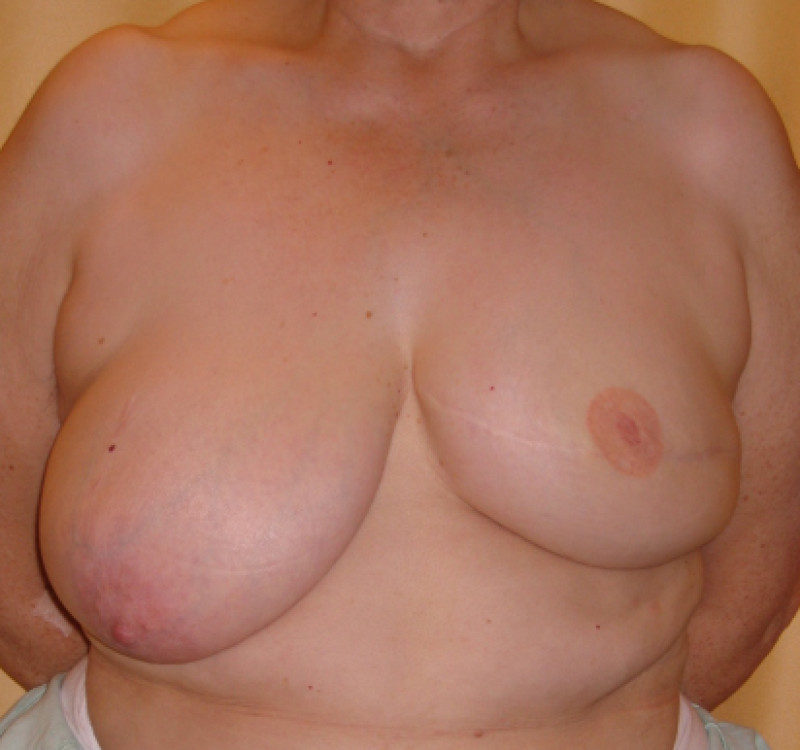
Fig. 3 Acceptable aesthetic result
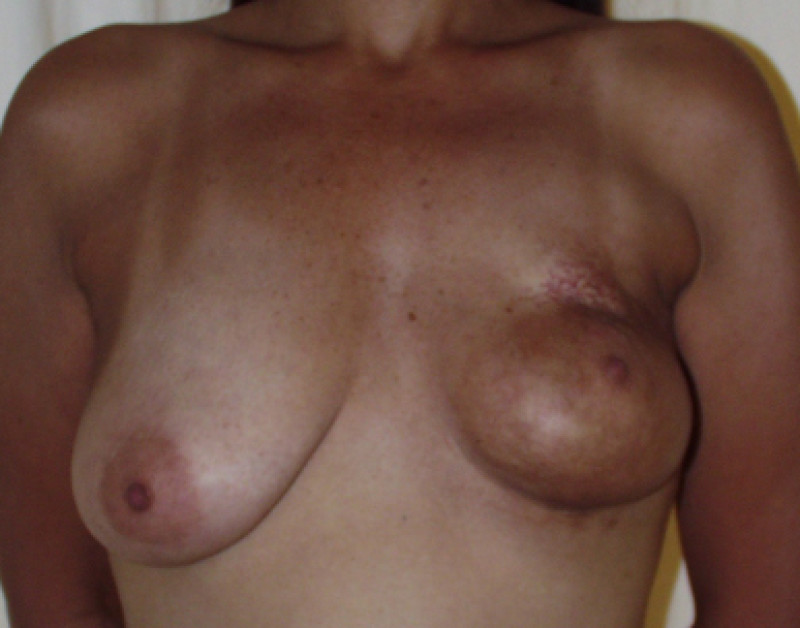
Fig. 4 Breast deformity
Assuming there are no contraindications, the decision on whether to undergo breast reconstruction should be entirely up to the individual. Outcomes of patients who undergo reconstruction, are similar in patients who choose not to. In addition, breast reconstruction patients do not have an increased risk of developing recurrence or metastases and will live just as long as non-reconstructed patients.
In our experience, patients dealing with the initial shock and fear of a breast cancer diagnosis, tend not to consider the aesthetic implications of treatment. They only realize the full impact of this with the passage of time, as the shock and fear subsides. Receiving information about breast reconstruction before undergoing surgery and having a simultaneous cancer resection and breast reconstruction, can give a superior aesthetic result, without reducing the effectiveness of the oncological treatment.
Every patient has a choice:
I prefer to have a surgical breast reconstruction
no, breast reconstruction is not for me, but I would like to know the other options available
Non-surgical solutions
A significant number of women with breast cancer decide not to have reconstruction. This can be for a variety of reasons; the patient is comfortable with the idea of living without her breast(s), or her partner or family are convinced that reconstruction is unnecessary. Unfortunately though, we frequently notice that this decision is based on inaccurate or incomplete information. Obtaining the correct information from peers, patient support groups, academic publications, relevant websites and medical personnel that are involved in breast cancer treatment, can help you make the right decision.
In breast cancer, complete oncological treatment always takes priority over the reconstructive procedure. This includes a swift and professional diagnosis, correct ablative surgery, adequate adjuvant therapy (radiotherapy, chemotherapy and hormonal therapy) and finally good out-patient follow-up. However, once the cancer treatment has been completed, you will be faced with the consequences of your oncological treatments and over time, the aesthetic aspects assume an increasing level of importance. Obtaining the correct information about breast reconstruction before starting treatment, and simultaneously addressing the oncological and aesthetic aspects, will result in a superior cosmetic outcome without influencing the quality of the oncological treatment or long-term prognosis.
An external breast prosthesis is one option (fig. 1). This is a teardrop shaped silicone device that can be added to a bra to imitate the breast shape. It can be worn either loosely, in a specially designed bra, or attached to the chest skin by an adhesive support. Different sizes and shapes are available. The external prosthesis can be a temporary solution whilst awaiting surgery or be a permanent device. The main advantage of an external prosthesis is that no additional surgery is required. The major drawback is that an external prosthesis has to be replaced every day and is sometimes difficult to combine with certain clothing. For many patients an external prosthesis remains a stigma, constantly reminding them of their breast cancer.

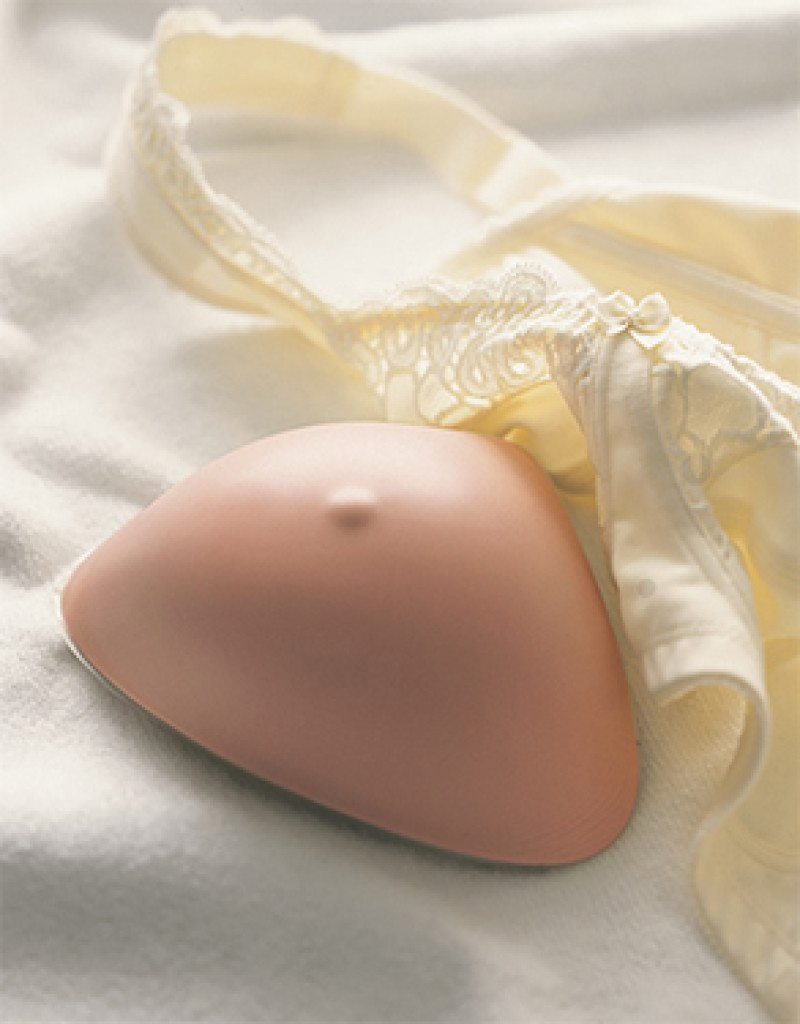
Fig. 1 external breast prosthesis
Some of the companies that offer external breast forms and provide more information include: www.amoena.com and www.anita.com
Benefits of an external prosthesis:
Artificially restores the natural shape of the breast.
Avoids further surgery.
The external prosthesis can easily be exchanged, if the volume of the other breast changes.
An external prosthesis is often reimbursed by public health care systems or private insurance companies.
Disadvantages of an external prosthesis:
Wearing low cut dresses or blouses can be more difficult than following surgical breast reconstruction.
The prosthesis may feel heavy, cold, or warm and sweaty, leading to skin irritation.
A loose prosthesis can move and sometimes slip out of a bra. It may be necessary to wear a special bra or adapted clothing to prevent this from happening.
Certain sports or hobbies can become more difficult, unless a specific support garment is worn, for example, a specially adapted swimsuit.
The volume of the prosthesis does not change with fluctuations in weight, although a different prosthesis can be bought.
An external prosthesis can be purchased in specialty lingerie stores or orthopedic shops. Get advice from personnel who specialize in measuring and modifying such prostheses.
Surgical solutions
The main goal of reconstruction is resumption of normal social and professional activities as quickly as possible after treatment for breast cancer. This primarily means being able to wear different styles of clothes without having to worry about the look or appearance of her breasts and in particular the décolleté area.
Following a mastectomy, breast reconstruction can significantly improve a woman’s self-image and self-esteem. She can again feel feminine, facilitating a return to normal sexual activity. The changing emotions of fear, dismay and depression may be dampened or even overcome.
Especially after a delayed reconstruction, a patient may also feel more attractive, helping her as a woman, wife and mother fulfill her different social roles and professional activities. In addition, with the passage of time, hopefully she will be reminded less and less about the initial treatment for cancer as a result of the improved appearance of her breast(s).
Some points worth considering about surgical breast reconstruction include:
Regardless of the type of reconstruction, you will have to undergo more surgery. This means more discomfort, with additional risks and possible complications.
You will be off work for longer and unable to attend to your family.
If you are unlucky enough to have a complication, it will take more time for you to recover.
There may be more scars.
With additional surgery, higher expenses may be incurred, depending on your personal insurance plan.
You need to have realistic expectations about the surgical results that can be achieved.
The reconstruction, no matter how good it is, will never replace your natural breast.
For implant based breast reconstruction, one should be aware that the longer the implant is in place, the more likely it is that complications may arise.
If you decide to proceed with surgical breast reconstruction, two more important issues have to be considered:
the timing of your breast reconstruction and the number of operations required
the surgical technique that suits you best
Timing of reconstruction
Knowledge about the timing of reconstruction is also important as several options are available.
Immediate or primary reconstruction is associated with a much lower psychological morbidity than delayed reconstruction. There are fewer operative procedures and anesthetics, together with a reduced hospital stay. This makes immediate breast reconstruction more tolerable for the patient and significantly less expensive. Several recent studies have indicated that there is no risk of delaying subsequent adjuvant therapy.
Delayed or secondary reconstruction is performed at least 6 months following the final adjuvant treatment (i.e. chemo- or radiotherapy). During this period, detailed information about the type of tumor, staging and prognosis are available and the patient has an opportunity to select her plastic surgeon, type of reconstruction and plan the procedure.
Tertiary reconstruction or reconstruction after previous failed attempts can be performed at any time depending on the condition of the local tissues.
Number of procedures
Regardless of the indications, technique or timing of breast reconstruction, the final result invariably involves more than one surgery.
Traditionally, transfer of some local or distant tissue is performed at the first operation to achieve as close a match as possible, in terms of both shape and volume, to the contra-lateral breast. We like to follow the classical principles of sculpture: a block of material, in this instance fat, is placed on a platform, the chest wall. The first operation is intended to create a “basic” shape by transferring a large piece of tissue. The tissue resembles a breast but the final shape and volume have not yet been established. An additional 10-15% of tissue is transferred to allow removal of smaller amounts of fat at a second procedure.
The second operation takes place approximately six months following the initial surgery. The transferred tissue has experienced the effects of gravity, acquired a new, more natural shape and is at its final resting position on the chest wall. Under local or general anesthesia, the second operation is then performed to improve the symmetry between both breasts. The majority of patients do need a second surgical intervention, as it is virtually impossible to obtain a perfect result after only one procedure. However, it is still sometimes possible to achieve a satisfactory result at one sitting. Symmetry is our main goal after the second procedure: it can be achieved by adjusting the reconstructed breast, adjusting the contralateral breast or a combination of both alternatives.
Alterations to the reconstructed breast include nipple reconstruction, scar revision (if required) and shape or volume adjustments. To adjust the volume, again following the classical principles of sculpture, we prefer to remove small amounts of fat and skin excess by relatively simple techniques, such as direct excision and/or liposuction, in preference to adding more tissue. The latter involves more complex techniques, such as local tissue transfer or lipofilling.
Adjusting the shape can be achieved by repositioning and/or rotating the flap. Skin resection and correction of the infra-mammary fold or other borders of the reconstruction, can also help achieve a more aesthetically pleasing result. More and more, small changes in shape can be achieved by less invasive techniques. For example, removing fat by liposuction at one place and adding that same fat to another area by lipofilling. This less invasive surgery also enables a patient to recover more quickly.
The other, natural breast can also be adjusted by augmentation, reduction or breast-lift (mastopexy). A prophylactic mastectomy with or without reconstruction may also be required.
In reality, it is not always easy to obtain perfect symmetry between both breasts and it may be necessary to repeat flap corrections or adjustments of the contralateral breast. These small “nip and tuck” procedures are tailored to each individual and can almost always be done under local anesthesia. They may need to be repeated until the patient is happy with the result, although their expectations must be realistic. The thoughts and opinion of the surgeon are obviously important but secondary to the wishes of the patient.
At a third operation, 3 months following the last corrective procedure, tattooing of the new nipple and areola is performed. Reconstruction of the areola with skin grafts is no longer done as the results are no better than following simple tattooing. As our eyes are very sensitive to colour differences, bilateral tattooing, even over the normal contralateral nipple-areola complex, provides the most natural results. Unfortunately though tattoos fade over time and may need to be repeated.
